If your dental hygienist cleans your teeth every six months or so, you know that a routine professional cleaning involves scaling teeth and the gumline to remove plaque and tartar, and polishing to remove stains and smooth the tooth’s surface. This is done to keep your teeth and gums healthy. If you have symptoms of gum disease, however, you may need another type of cleaning, called scaling and root planning.
Whether you call it deep cleaning, or root planning and scaling teeth, this conservative procedure plays a critical role in treating periodontal disease. So, if your dentist recommends scaling and root planning for you, rest assured it’ll put you on the road to good periodontal health.
With the combination of our daily meals and drinks, natural accumulation of dental plaque can build up on our teeth. While regular brushing can help remove this, it can harden into tartar if left untouched and lead to a variety of dental health complications including gum disease and tooth decay. Below, we’ll discuss the procedure of scaling and root planning, symptoms, warning signs, and the deep cleaning of teeth side effects.
When Is Scaling and Root Planning Recommended?
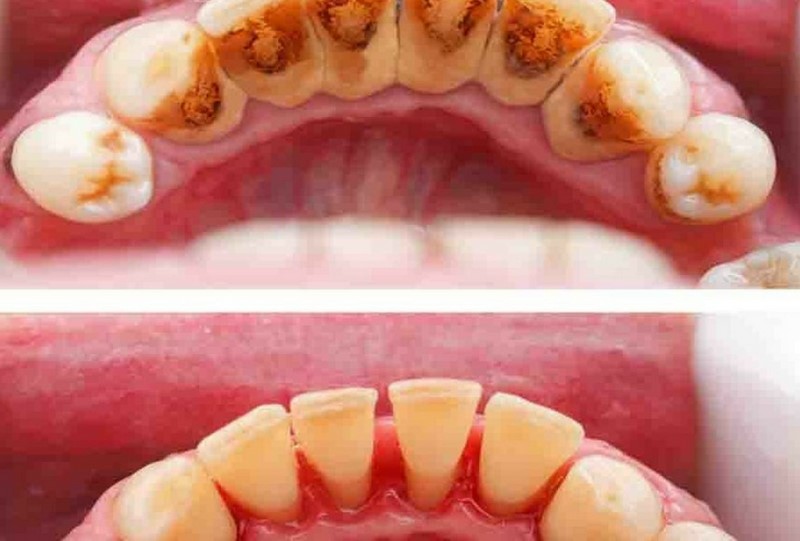
Although routine cleanings are done to prevent periodontal (gum) disease, scaling and root planning is a non-surgical procedure done to treat periodontal disease. In fact, this procedure – sometimes called a deep cleaning – is considered the “gold standard” of treatment for patients with chronic periodontitis.
Healthy gum tissue fits tightly around each tooth, and it is recommended the measurement from the top of the gumline to where it attaches to the tooth should only be 1 to 3 millimeters in depth. But, when bacterial plaque and tartar accumulate around and under the gums, tissues that support your teeth may be affected and periodontal disease can develop causing deeper pockets to form.
When you have more advanced signs of gum disease (bad breath, heavy tartar buildup and unhealthy pocket depths of 4mm or more), your dentist may recommend scaling and root planning as the first procedure necessary to treat the condition.
Why Is It Important?
The process of periodontal scaling and root planning is far more comprehensive than your average routine teeth cleaning. Gum disease can start off minor before quickly progressing into a painful, damaging situation. Seeing a dentist regularly can help identify early signs of gum disease that can often be treated with a simple cleaning. However, untreated gums and teeth require the deep cleaning process of a scaling and root planning.
Signs and Symptoms
Following the deep cleaning, instruments are used to plane or smooth out all of the root surfaces. These techniques help the gums reattach to the roots of teeth and to reduce long-term gum issues like bleeding and inflammation.
As with most medical procedures, it’s important to note that there may be some symptoms immediately following scaling and root planning. It’s important to anticipate these symptoms and to know how to maintain your gums post-procedure.
Here as some common symptoms that patients experience:
Tooth Sensitivity
You may feel a new sensitivity to temperature changes and/or sweet food and drinks. The sensitivity to temperature may be particularly acute for the first two or three days following treatment. In some situations, it may take a few weeks before all sensitivity disappears
Bleeding
This temporary sensitivity will extend to your gums and you might experience some slight bleeding during brushing immediately following the procedure. This bleeding should decrease and then ultimately cease within three days.
Discomfort and Pain
Many patients ask us if scaling and root planning is painful and the answer is that there can be discomfort. The procedure does sometimes require the use of a local anesthetic. If so, it’s important to avoid chewing any foods or gum until full feeling returns to avoid injuring your numbed tongue and cheeks. Until you have fully feeling, avoid eating any sticky, hard, brittle, spicy, or acidic foods.
Risks of Scaling and Root Planning
Root planning and scaling can introduce harmful bacteria into the bloodstream. Gum tissue is also at risk of infection. You may need to take antibiotics before and after surgery if you have a condition that puts you at high risk for a severe infection or if infections are particularly dangerous for you. You may need to take antibiotics if you:
- Have certain heart problems that make it dangerous for you to get a heart infection called endocarditis.
- Have an impaired immune system.
- Had recent major surgeries or have man-made body parts, such as an artificial hip or heart valve.
The Scaling and Root Planning Procedure
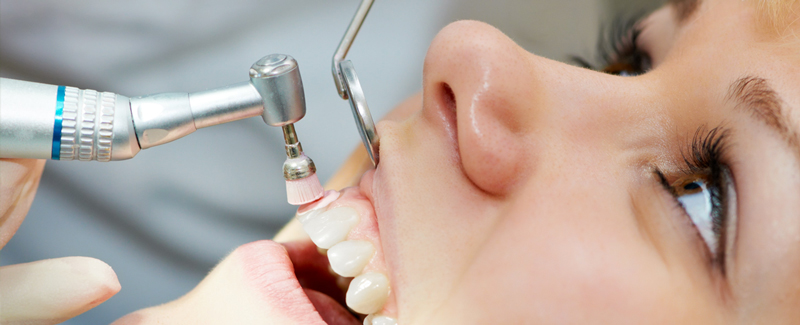
During the initial examination, a dental hygienist and/or general dentist will evaluate your plaque buildup and examine your gums for possible periodontal problems. Using an instrument called a periodontal probe, the depth of the spaces between your teeth and gums, called the sulcus) will be measured. At the edge of the gumline, healthy gum tissue forms a sulcus; a shallow, v-shaped groove between the tooth and gums. Normal sulcus depth is 3 mm or less. With periodontal diseases, the sulcus widens, creating a deeper pocket of more than 3 mm, resulting in harmful plaque buildup that cannot be cleaned without professional dental treatment.
Scaling and root planning is performed when pockets are greater than 3 mm. Scaling removes plaque and tartar above and below the gumline. Depending on the amount of tartar and plaque buildup, and your level of tooth sensitivity, tooth scaling may prove painful; a numbing gel or anesthetic injection typically will be administered to the area to lessen discomfort.
Once numbing or anesthesia is achieved, your dental professional will use an instrument called a small scaler, an ultrasonic cleaner, or both to thoroughly remove plaque and tartar to the bottom of each periodontal pocket. The tooth surfaces then are planed – or smoothed – which prevents plaque from accumulating along root surfaces and allows gum tissue to heal.
Depending on the severity of your condition, scaling and root planning may be performed quadrant by quadrant to ensure comfort. Typically, the upper and lower quadrants on one side of the face are done at one appointment, and the upper and lower quadrants of the other side are done at a second appointment.
At the treatment appointment, your dentist also may administer local antibiotics, antimicrobials and other medications directly into the periodontal pockets to help control infection or pain, as well as encourage faster healing.
Early stage gum disease treatment may include tooth scaling and cleaning at three-month intervals, as well as the use of medicated mouthwash and daily flossing. Later stage gum disease treatment may include deep plane scaling, periodontal surgery and laser surgery.
Dental Lasers for Scaling and Root Planning

Using dental lasers during periodontal therapy typically results in less bleeding, swelling and discomfort during surgery. However, periodontal tissue damage may occur if inappropriate laser wavelengths and/or power levels are used during the periodontal procedure. Therefore, it is very important that only dental professionals trained and experienced in the proper and safe use of lasers perform this adjunct laser procedure.
After the Procedure
At a follow-up visit, your dentist will want to check on the healing of your gums and the status of your pockets. The good news is that in most cases, red or swollen gum tissue becomes firm and pink again, bleeding is reduced or eliminated and pockets get smaller. If your gum tissue has responded well and remains stable, you may not need any further treatment.
More advanced periodontal conditions, on the other hand, may require surgical interventions by a periodontist after root planning and scaling to stop the progression of bone loss. However, your scaling and root planning treatment often lessens the amount of surgery you need.
After-care and Recovery
For the first few days after scaling you may experience some bleeding that should gradually subside. At a follow-up appointment, your dentist will evaluate gum healing and verify a decrease in the size of periodontal pockets. If pockets greater than 3 mm are still present after initial treatment, additional treatment may be recommended.
Maintaining good oral hygiene practices and continued, long-term follow-up by your dental professionals are essential to prevent periodontal disease from developing into a more serious and/or chronic condition that may require surgery. This is important, especially given the growing body of clinical evidence indicating the strong connection between periodontal disease and secondary health conditions such as cardiovascular disease, low birth weight babies and premature births.
Homecare Tips to Reduce Symptoms and Hasten Healing
Rinse Regularly
Use either an antimicrobial mouthwash or a warm saline rinse 2 to 3 times a day for the first week following treatment. Once you have returned to normal, use of such rinses should be limited to once a week.
Use a Desensitizing Toothpaste
 Extreme tooth sensitivity may tempt you to ignore your regular brushing habits. This can bring on other tooth and gum issues. You can keep the good habits without the pain by using a special desensitizing toothpaste containing potassium nitrate.
Extreme tooth sensitivity may tempt you to ignore your regular brushing habits. This can bring on other tooth and gum issues. You can keep the good habits without the pain by using a special desensitizing toothpaste containing potassium nitrate.
Rethink Your Diet
Implement a diet of softer foods, such as steamed vegetables and soups, until all the above symptoms cease.
Oral Care for Prevention
Periodontal disease can sneak up on you without warning, and the doctors urge you to follow through with regular dental checkups and periodontal examinations. A good home care routine is key in preventing gum disease from starting and keeping your mouth healthy after any type of oral treatment. Here’s what you need to do:
- Brush at least twice a day with a fluoride toothpaste.
- Replace your toothbrush when the bristles are worn.
- Floss daily to clean between your teeth and bridge work, crowns or implants.
- Use an antimicrobial mouthwash.
- Don’t smoke! Or if you are a smoker, please try to stop smoking to make your body healthier.
Additional Considerations
For maximum patient education and protection, it is important to note certain distinctions. “Polishing” involves smoothing a surface; “cleaning” involves removing waste and other extraneous particles from teeth. Oral prophylaxis commonly is defined as removing plaque, calculus and stains from the exposed and unexposed tooth surfaces by scaling and polishing. The prophylaxis procedure is performed on a healthy mouth to prevent periodontal disease. Polishing-only procedures are considered cosmetic and have no therapeutic value. While many patients may equate polishing with oral prophylaxis, it is a mistake to assume that tooth polishing alone constitutes preventive oral health care.
Scaling and Root Planning Costs
Factors affecting the cost of gum disease treatment include the technology used in the procedure; the dentist’s location; type of dental insurance; type and frequency of treatment and follow-up care; and type and number of dental professionals involved in the treatment plan. For example, your general dentist may perform the initial diagnosis and some treatment, but may refer you to a periodontist more adept at performing advanced surgical procedures.
